Learning About Non Hodgkin Lymphoma
- Lee Troutman, is feeling “stronger than ever” after being diagnosed at 20 years old with a rare disorder called Hemophagocytic Lymphohistiocytosis (HLH) and late-stage non-Hodgkin’s lymphoma just months later.
- Now, in remission, Troutman, who initially likened his cancer symptoms to “working too much,” is sharing his story and urging others to stay strong amid difficult times.
- Lymphoma is a type of blood cancer. Blood cancers can affect the bone marrow, blood cells, lymph nodes and other parts of the lymphatic system.
- It’s important to note there are more than 40 different types of lymphoma. Hodgkin lymphoma and non-Hodgkin lymphoma are the main two sub-categories with the latter being more common. Diffuse large B-cell lymphoma (DLBCL), the one Troutman battled, is the most common form of lymphoma.
Now, 22, the inspirational young man, who is in remission and back to living life as he once new it, is sharing his story of hope.
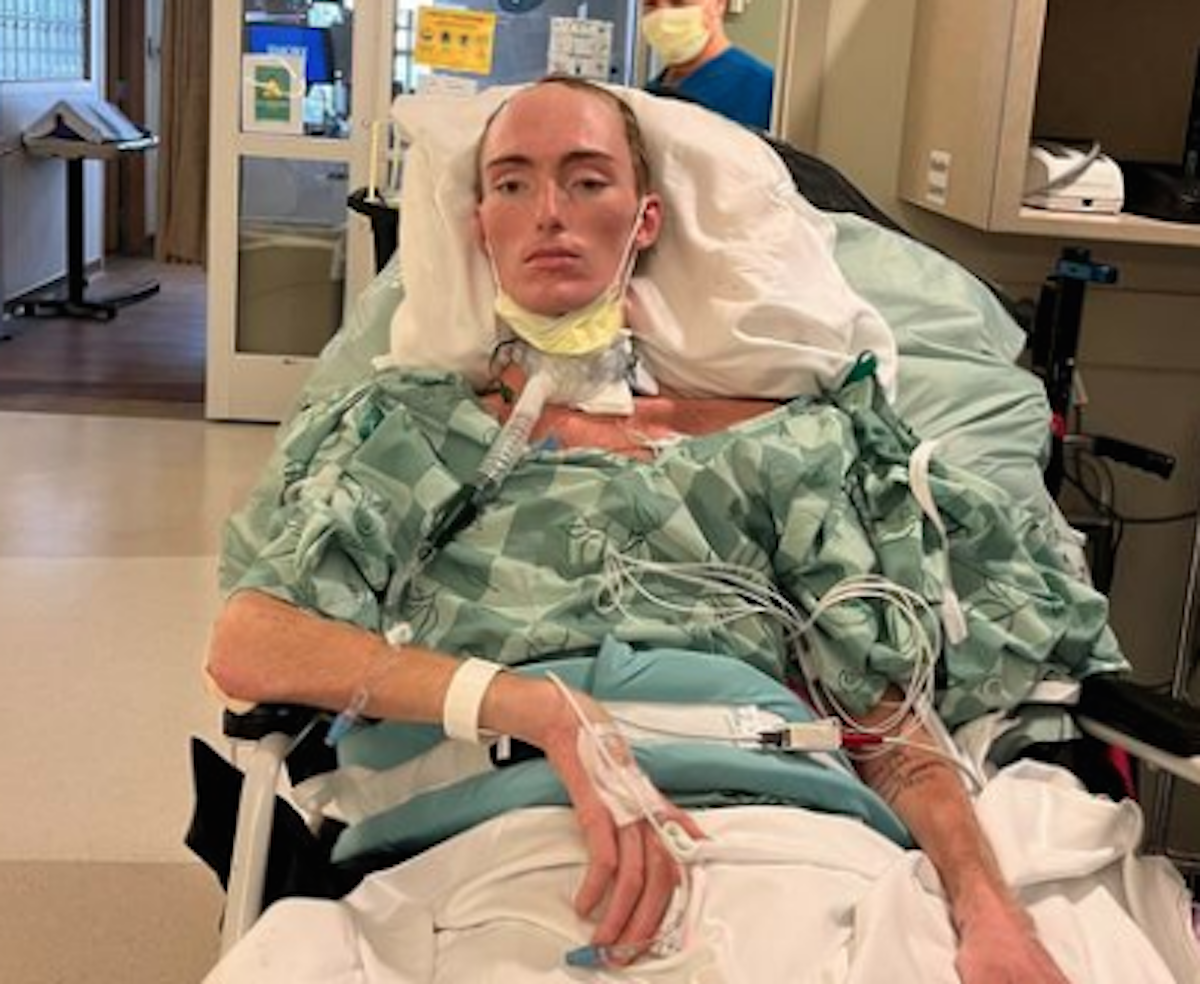
He explained further, “But once I was diagnosed, things rapidly got worse — my eyes and skin were going yellow from my liver failing. I couldn’t walk, talk, eat — anything.
“Nor was I really aware of what was going on; I wasn’t in a coma but my mind was constantly fuzzy.”
Months after learning he had HLH — described as “a rare but potentially fatal condition in which certain white blood cells (histiocytes and lymphocytes) build up in and damage organs” by the Dana-Farber Cancer Institute — doctors informed Troutman he had non-Hodgkin’s lymphoma, which had spread to his spin, liver, ribs, hips, his brain stem, and four lobes of his brain.
Troutman first sought medical advice from his doctor in October 2021. One month later he was diagnosed with mononucleosis (a viral infection). He received his HLH diagnosis in December 2021, followed by his lymphoma diagnosis in January 2022.
“The doctors did not think I would survive. My mom and I found a doctor who agreed to take my case, he gave me hope with a 5% chance of survival,” the determined young man recounted.
“He said if I was to survive the lymphoma and aggressive cancer treatments, I would then need a bone marrow transplant. And after that, I would have a 70% chance of making it through.”
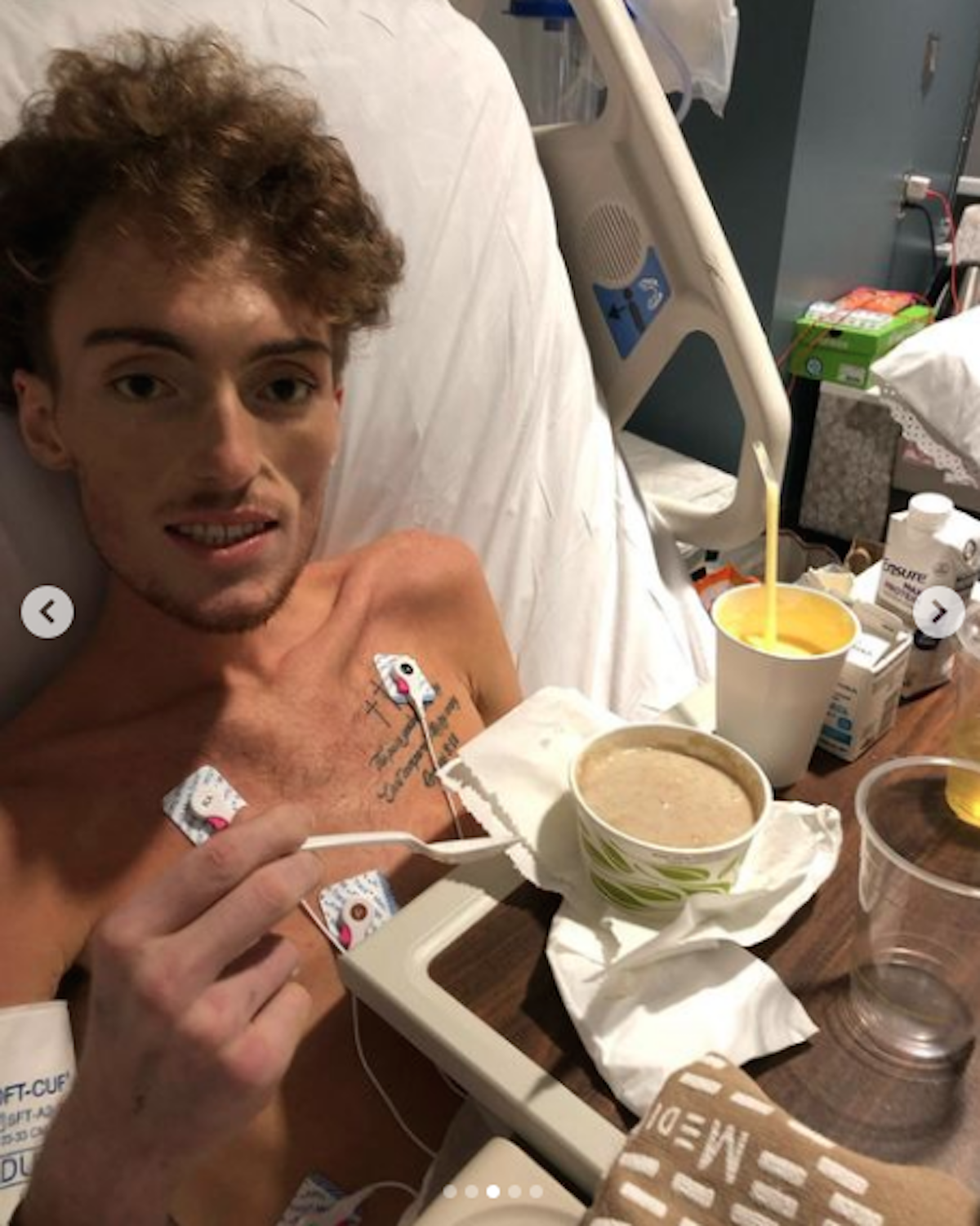
Throughout all that Troutman dealt with amid his cancer journey, he never gave up. Even when his lungs collapsed, twice, prior to having a bone marrow transplant. He ultimately ended up on a ventilator with a feeding tube until he was ready to rehabilitate — a process which took months.
“The goal was to get me strong enough to withstand the bone marrow transplant. During this time, I re-learned how to do pretty much everything, from walking to eating. I also received more than 50 platelets and blood transfusions,” he explained.
“I had too many chemo treatments to count and multiple radiation treatments on my brain. At the time I didn’t remember the treatments but looking back it’s overwhelming. I definitely have some PTSD which I speak to a counsellor about regularly.”
He ultimately received a bone marrow transplant on May 24, 2022, which followed a lengthy quarantine period and taking dozens of drugs to prevent his body from rejecting the transplant or HLH recurrence.
Despite all that he’s been through, Troutman regularly, and confidently, posts on social media to show how far he’s come.
“I am living my best life, working out at the gym again, I have a job and I am finally looking forward to my future,” he said, according to The Mirror.
“If there is anyone out there going through something similar, stay strong, keep fighting, and do not give up. If the doctors have given up, go find a new doctor. Be your own advocate.”
Earlier this year, Troutman shared footage of himself during his recovery period, also expressing how “blessed” he is to be alive.
More Inspiring Stories About Resilience & Being Your Own Advocate
- Resilience: Staying Positive Despite Adversity
- The Power Of Prayer: The Remarkable Link Between Religion And Resilience
- Michael J. Fox’s Determination to Remain Positive During Decades-Long Parkinson’s Journey Shows Cancer Patients the Importance of Optimism
- Be Pushy, Be Your Own Advocate… Don’t Settle
He captioned the post, “Mom sent me these videos today. I’ve never seen these but I felt like I needed to share them to show y’all what I went through. Very tough but I did it god did it. I wouldn’t be here today if it wasn’t for Mom and Dad and Lily’s support. Steven also helped.
“Again I’m so blessed to be here because they said I was supposed to die, Never a good feeling. Again I love live life to the fullest now. Everyday I wake up now is a blessing.
“One thing I learned is that never take things for granted, I’m not talking about objects I’m talking about family. Your family should be the most important thing in you life. Already I’ll be done typing because if I kept typing I think I might need 100 more pages. I love y’all!!! I love my self. I love family.”

Understanding Lymphoma
Lymphoma is a type of blood cancer. Blood cancers can affect the bone marrow, blood cells, lymph nodes and other parts of the lymphatic system. The Leukemia & Lymphoma Society reports that every 3 minutes, one person in the U.S. is diagnosed with a blood cancer.
More specifically, lymphoma is a cancer of the immune system that begins in the white blood cells called lymphocytes. Lymphoma begins when lymphocytes develop a genetic mutation that makes them multiply much faster than normal. This mutation also forces older cells that would normally die to stay alive. From there, the quickly multiplying lymphocytes collect and build up in your lymph nodes, the small glands in your neck, armpits, and other parts of your body.
What Kind of Lymphoma Do You Have? Why Your Type Matters
It’s important to note there are more than 40 different types of lymphoma. Hodgkin lymphoma and non-Hodgkin lymphoma are the main two sub-categories with the latter being more common. Diffuse large B-cell lymphoma (DLBCL) is the most common form of lymphoma.
The type of white blood cells linked to the disease determines the distinction between Hodgkin lymphoma and non-Hodgkin lymphoma. If doctors are unable to detect the Reed-Sternberg cell, giant cell derived from B lymphocytes, then the cancer is categorized as non-Hodgkin lymphoma.
You might be at a higher risk for lymphoma if you:
- Have been infected with the HIV or Epstein-Barr virus
- Had an organ transplant
- Have a family history of lymphoma
- Have been treated with radiation or chemotherapy drugs for cancer in the past
- Have an autoimmune disease
Signs of Lymphoma
One thing to note about lymphomas is this type of cancer often creeps in quietly, without symptoms. And even when symptoms do show up, they don’t necessarily point directly to cancer. In a previous interview with SurvivorNet, Dr. Elise Chong, a medical oncologist at Penn Medicine, explained that lymphoma symptoms could be difficult to detect.
Sneaky Lymphoma Symptoms Often Lead to a Late Diagnosis
“The symptoms of lymphoma, especially if you have a low-grade lymphoma, often are no symptoms,” Dr. Chong explained. “People say, but I feel completely fine, and that’s very normal.”
People with lymphoma do not always have symptoms, but common signs are:
- Swollen glands in your neck, armpit or groin
- Fever
- Chills
- Night sweats
- Unexplained weight loss
- Feeling tired
- Swelling in your stomach
No matter what, it’s important to communicate anything unusual happening to your body with your doctor. Even if there’s nothing to worry about, it’s good to rule out the possibility of more serious issues.
Learning About Diffuse Large B Cell Lymphoma
According to Lee Troutman’s Caring Bridge page, the type of non hodgkin lymphoma he was battling was called Stage Four Diffuse Large B Cell Lymphoma.
About 1 in 5 people with non-Hodgkin lymphoma have the diffuse large B-cell variety in the U.S. This is a fast-growing cancer, but when caught early, treatment success rates are high.
RELATED: What Does It Mean to Have Advanced-Stage Lymphoma?
“We never claim a 100% success rate in oncology, because we don’t have it, and nothing’s 100% in this world other than taxes and death,” Dr. Stephen Schuster, medical oncologist at Penn Medicine, tells SurvivorNet.
But, he adds, “diffuse large B-cell lymphoma in the early stage is a highly treatable disease.”
When Caught Early, Diffuse Large B-Cell Lymphoma Is Highly Treatable
According to the National Library of Medicine, “Diffuse large B cell lymphoma (DLBCL) is the most common lymphoma, accounting for about 25% to 30% of all the non-Hodgkin lymphomas. It typically presents as a rapidly growing mass or enlarging lymph nodes in a nodal or extranodal site.
“Though aggressive, they do respond well to six cycles of rituximab along with cyclophosphamide, doxorubicin, vincristine, and prednisone (R-CHOP).”
Determining Which Treatment Will Work Best Against Your Cancer?
Once the work of determining your type of cancer is finished, your doctor can focus on the next important step — how to treat you. If you have an indolent cancer and you don’t have any bothersome symptoms, you may not need treatment right away, Dr. Jennifer Crombie, medical oncologist at Dana-Farber Cancer Institute, previously told SurvivorNet.
Non-Hodgkin Lymphoma Treatment: Finding the Right Fit for You
If your cancer is more aggressive, whether it’s T-cell or B-cell, you can expect to get chemotherapy. Chemo may be part of a cocktail of drugs that are given in combination. These drugs work synergistically, going after your cancer in different ways to treat it more effectively.
Sometimes radiation therapy is used together with chemotherapy. Radiation uses high-energy x-rays to eliminate cancer cells. The radiation typically given for non-Hodgkin lymphoma is delivered from a machine outside the body, which is called external beam radiation.
One more thing your doctor will want to investigate is your cancer’s genetic makeup. Using a sample of your cancer cells taken during a biopsy, your doctor will test for genetic mutations and other abnormalities.
In some people with non-Hodgkin lymphoma, genes have swapped places, which doctors refer to as translocations. C-MYC, BCL2, or BCL6 are three common translocations. Having one of them could affect how your cancer spreads, and how well you might do in the future. Translocations can also change the course of your treatment.
“If patients have those translocations, sometimes we give a slightly different version of chemotherapy,” Dr. Crombie tells SurvivorNet.
‘Exceptional Responders’
If you’ve decided to enter a clinical trial and are wondering what kind of result you can expect, you should know there are a number of ways to answer this question.
RELATED: An Immunotherapy Breakthrough: The Judy Perkins Story
You should ask your doctor, or whoever is running your trial, for the data they have so far on the outcome of the treatment they’re testing.
Why Do Some People Respond Better to Treatment?
You should also ask whether there have been other people in the trial who have had a particularly positive response. They call these exceptional responders.
It’s, of course, something of an excruciating question, why some people respond to treatments better than others. In many cases, oncologists are still trying to figure out the answer to this.
However, simply being able to ask the question may well help you make a better decision if you’re looking at a clinical trial.
Clinical Trials Can be Life-Saving for Some
Contributing: SurvivorNet Staff
Learn more about SurvivorNet's rigorous medical review process.

